Need to know: COVID-19
- As of 11 a.m. on Friday, April 10, there were 3,908 confirmed cases in 91 counties in North Carolina with 74 deaths.
- As of April 8, projections from the Institute for Health Metrics and Evaluation (IHME) out of the University of Washington estimate North Carolina’s peak resource use will be on April 15 and that North Carolina will have enough hospital beds and ICU beds available at that time.
- The latest U.S. Department of Labor report shows another 6.6 million people filed for unemployment last week, with 137,573 of those in North Carolina (down roughly 34,500 from the previous week). From March 17 to April 7, North Carolina has seen 413,930 COVID-19 related unemployment insurance claims.
- On April 8, North Carolina received approval from FEMA to provide housing alternatives (motels, hotels, dorms) for those without stable housing who need to quarantine or are at high-risk of exposure.
- Essential workers who are parents and have no other child care options can apply for financial assistance through NC DHHS.
- North Carolina is following CDC recommendations that people with mild symptoms should stay home and call their doctor to decide if they need a test. Check out this fact sheet from NC DHHS on what to do if you feel sick.
For more, EdNC.org is updating this article daily with news and resources. All daily updates are archived at the bottom of the post.
Policy challenge: The disproportionate impact of COVID-19 on black communities
Over the past month, many have warned that COVID-19 would hit black and poor communities the hardest, and now we are seeing confirmation of that as some states release data broken down by race/ethnicity.
In North Carolina, black or African American people make up 39% of laboratory-confirmed cases and 38% of deaths from COVID-19 as of Thursday, April 9, despite making up an estimated 22% of the state’s population. You can see COVID-19 data broken out by race/ethnicity in the table below from NC DHHS.
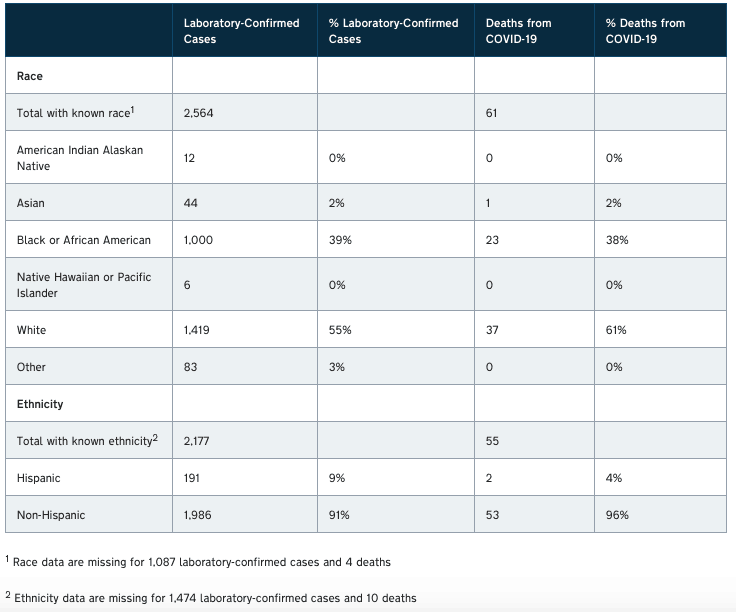
The data is even more stark in Louisiana, where black people make up 70% of deaths from COVID-19 despite making up about a third of the population.
Why is this happening? Several news outlets have published good explainers this week, including this article from North Carolina Health News and the featured article below by a UNC epidemiologist. In short, the virus is exposing longstanding disparities in access to health care and health insurance, jobs that allow for social distancing and provide paid sick leave, adequate housing, and basic resources for health and well-being.
UNC epidemiologist Grace Noppert summed it up this way: “It is evidence of centuries of segregation and discrimination that have disproportionately placed people of color in communities without access to health care, with degraded and crowded living conditions and a lack of basic opportunities for health and wellness.”
And a recent New York Times article quoted NC DHHS Secretary Dr. Mandy Cohen, saying: “This current crisis lays out what we have known for a long time, which is that your ZIP code is often a determinant of your health outcome.”
In terms of policy solutions, this is a systemic issue that will not be solved overnight. However, releasing data by race/ethnicity is the first step in understanding how the virus is impacting our communities and what can be done in response.
What we're reading
COVID-19 is hitting black and poor communities the hardest, underscoring fault lines in access and care for those on margins
UNC epidemiologist Grace Noppert explains why we are seeing data this week showing that COVID-19 is disproportionately impacting black communities across the country. ... Read the rest-
Our fragile child care ‘system’ may be about to shatter
-
New Coronavirus Drug Shows Promise in Animal Tests
-
Small, Mid-Sized Cities Currently Cut Out of Direct Coronavirus Funding
-
Facebook lends more data to the coronavirus fight
-
After the Pandemic: Addressing the Permanent Crisis With Pay for Success Programs
-
Everyone will be learning differently for a while — but what about students with learning differences?